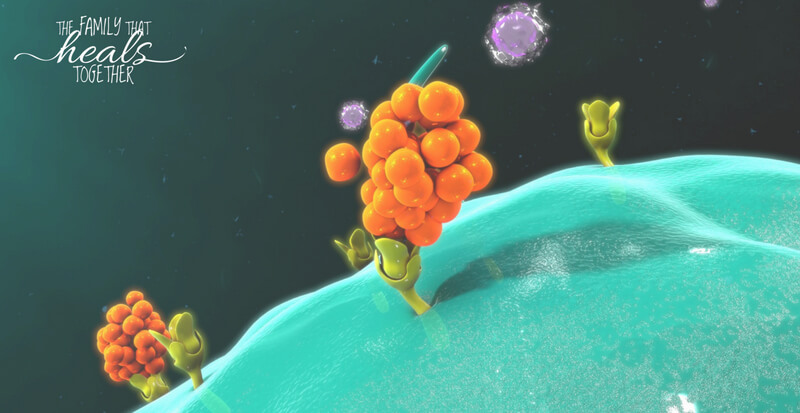
Ever heard of a cytokine storm? It’s sort of a mysterious blanket term for periods of high inflammation that those with chronic illness sometimes experience. Below, Danielle breaks down the cytokine storm, explaining inflammatory cytokines and how they affect the body.
What are cytokines and how do they work?
A cytokine storm involves cytokines: tiny protein molecules that signal the cells around them. Examples of cytokines include:
- Interleukins
- Leukocytes
- Lymphokines
- Chemokines
- Interferons
- Tumor necrosis factors
Many cells in the body produce cytokines, even other cytokines!
Similar to cytokines, hormones signal other cells. However, hormones regulate overall body and organ functions, whereas cytokines are the messengers of the immune system.
Cytokine messengers are released from one cell and then received on receptors of nearby cells, creating a domino effect of help or harm.
Scientists discovered the first cytokines in 1957 and called them interferons because of their ability to “interfere” with viral replication. Since then, a number of cytokines have been found. For example:
- Lymphokin- released from immune cells, lymphokines turn “on” or “off” other parts of the immune system. Essentially, sending smoke signals to other immune cells to mount an attack against an invader.
- Interleukins- produced by leukocytes, interleukins regulate your immune response. In labs tests, interleukins matter. Low levels have been found in those with autoimmune disease and low immune illness.
- Leukocytes- floating around in the blood and battling foreign invaders, leukocytes include macrophages, monocytes, lymphocytes, granulocytes. When your doctor suspects an infection, be on the lookout for high leukocyte numbers.
But, don’t get bogged down in all the “cytes.”
Cytokines are simply regulators that manage your body’s response to anything that shouldn’t be there: trauma, immune issues, inflammation, and infection.
Anti-inflammatory vs. inflammatory cytokines
Just like everything in the body, cytokines can be good or bad, anti-inflammatory or pro-inflammatory.
What’s more, all cytokines have the potential to express signals for health or disease, even if they traditionally belong in one camp.
This is because cytokines have the ability to stop or start inflammation, managing things like pain, fever, tissue repair and break down, and blood cell production.
And for better or worse, cells will keep replicating the messengers as they roam about.
What do pro-inflammatory cytokines do?
Interleukins (IL-1) and tumor necrosis factor (it just sounds awful – TNF) are pro-inflammatory cytokines, meaning they signal your body to continue allowing and creating inflammation.
These cytokines cause fever, inflammation, tissue deconstruction, and even death.
You can trace many pathological pain diseases to overactive pro-inflammatory cytokines.
What is a cytokine storm?
Just like any storm, a cytokine storm builds if left unchecked. More pro-inflammatory cytokines lead to even more inflammation, causing a domino effect, or the perfect storm… of pain.
Cytokine overproduction may keep your body in a constant state of inflammation which leads to even more inflammation.
Cytokines have a large role to play in an overactive immune response. Overactive immune reactions to infectious and noninfectious diseases can cause high fever, swelling, nausea, and fatigue. These are called cytokine storm symptoms, or CSS.
Macrophages from the initial inflammation activate a cytokine storm. Things like inflammatory foods, a negative outlook, emotional abuse, or lack of sleep will all feed the cytokine storm and keep the body inflamed.
Let’s talk about what cytokines have to do with chronic and acute health conditions, pain, inflammation, trauma, and mental health.
Overactive inflammatory cytokines play a role in chronic pain conditions, including fibromyalgia, lupus, MS, and more.
Cytokines trigger disease to persist by releasing signals in the nervous system and a cytokine storm perpetuates inflammation. This can even happen in your brain, where depression and anxiety may be the result of active inflammatory cytokines.
If the body experiences an intense bout of harm but has reserves to heal itself, the cytokine reaction will only last for a short period of time. The body will have what it needs to heal and not allow cytokines to get out of control, causing constant inflammation.
However, if the body feels low on reserves and experiences intense pain – or experiences it for a long period of time – the body’s energy reserves cannot fight the inflammation cascade.
This explains why cytokine storms are seen in chronic illness and pain sufferers, and not often in those without inflammation.
Again, the domino effect of the cytokine’s synergistic communication spreads more inflammation.
How to quiet a cytokine reaction
If you find yourself in a cytokine storm, adjusting your diet and lifestyle may be enough to calm the symptoms. However, if you have severe CSS, you may be a candidate for CSS treatments which block the production of pro-inflammatory cytokines.
But it’s important to address the root cause before treating with cytokine blockers, as they could make the condition worse.
For example, in the case of sepsis, cytokine blockers may support the spread of infection. But on the flip side, cytokine blockers also effectively manage IBS and rheumatoid arthritis. Cytokine blockers might also help with chemotherapy side effects, as many use anti-histamines (a type of cytokine blocker) to combat side effects.
There are also natural cytokine blocking supplements like this one that may help.
The biggest concern when using cytokine blockers is that they will interfere with the immune system’s ability to fight the foreign invader. For that reason, you may want to consider treating chronic pain with lifestyle changes, rather than conventional CSS treatments.
Lifestyle changes to calm a cytokine storm
Anti-inflammatory foods help calm a cytokine storm. This includes foods like wild blueberries, turmeric, green tea, celery, beets, and green leafy vegetables. Other foods slow the inflammatory messengers, such as organic fruits and vegetables, grass-fed meats, and bone broth.
If you have an advanced cytokine storm, inflammation, or autoimmune disease, you may want to go beyond single foods and transform your whole diet. Consider the GAPS diet or an autoimmune paleo (AIP), keto, or paleo diet.
Fortunately, with lifestyle changes, even the worst cytokine storm can be quelled.
Your lifestyle plays a huge role in cytokine expression. These steps can help tame the storm:
- Exercise regularly. Exercising at least two to three days per week can calm pro-inflammatory cytokines and greatly lessen pain. This includes walking, pilates, weight lifting, or whatever you enjoy.
- Cut out inflammatory foods. Such as gluten, dairy, conventional meats, nightshades, oxalates, and legumes. If you experience serious pain, consider the GAPS diet to lower inflammation.
- Be sure to drink at least 8 glasses of filtered water daily. In the middle of a detox? Drink more!
- Get at least 8 hours of sleep each night. (Read about how to improve your sleep here.)
- Stimulate your vagus nerve and laugh, meditate, pray, or sing daily!
- Get rid of negative thoughts. Instead, focus on positive affirmations or Bible verses daily.